Care Management, Always Connected

Care management works. A dedicated professional who stays connected to a health plan member over time — not just during acute episodes — reduces hospitalizations and lowers costs, cuts avoidable ER visits, and reduces 30-day readmission risk by as much as 32%. Beyond the metrics, care managers do something harder to quantify: they translate the healthcare system for people overwhelmed by it. They answer the question a member didn't know to ask. They notice when something is off.
That relationship is the active ingredient. Everything else is infrastructure.
The problem is bandwidth, not intent
But the model that makes care management effective is the same thing that limits it. Contact frequency directly predicts outcomes, yet the CMS baseline for chronic care management is just 20 minutes per member per month. Members get a call once a month, sometimes less. Between those calls, they're on their own.
That gap matters. Within 30 days of discharge, roughly one in five members experiences an adverse event — most commonly medication-related, and most preventable. Poor medication adherence is a significant predictor of 30-day readmission. And a randomized study of telephonic care management for Medicaid beneficiaries found no significant improvement in hospitalizations or ER visits, attributing the result directly to difficulty maintaining engagement between calls.
The model is right. The bandwidth isn't there.
Digital health filled part of the gap — but missed the relationship
The natural response has been technology: member portals, apps, automated outreach, SMS reminders. These tools have real value — mobile health apps improve outcomes in chronic conditions like diabetes. But they're designed to help the member manage themselves. The member is the operator; the technology is the interface.
That's meaningful — but fundamentally different from care management. And the engagement data reflects it. Studies consistently report high dropout rates and low sustained adherence as central barriers, with retention remaining a persistent challenge across populations.
The members who need the most support are often the least likely to open an app — not because the technology failed, but because self-management tools can't replicate someone who knows you, checks in on you, and connects you back to your care team when something shifts.
The care manager's reach, extended
Conversational AI changes the equation — not by replacing the care manager, but by extending their presence into the time between sessions.
Where a digital health app asks members to manage their own condition, a conversational AI agent works on behalf of the care manager. It reaches out. It checks in. It asks how the member is doing — not in a generic push notification, but in a natural conversation that feels like a call from someone who knows their situation. Everything it learns flows back to the care manager, so the next human interaction starts in context.
Consider what this looks like in practice. A care manager wraps up a session with a member struggling with depression and medication adherence. The next call is two weeks away. The AI agent reaches out three days later — a brief check-in. It asks how the member has been feeling, walks through the PHQ-2. The member scores higher than last time. Something has shifted.
The agent flags this immediately. The care manager calls that afternoon — already in context, already knowing what changed. Without the agent, that shift goes undetected for eleven more days. With it, the care manager intervenes the same day.
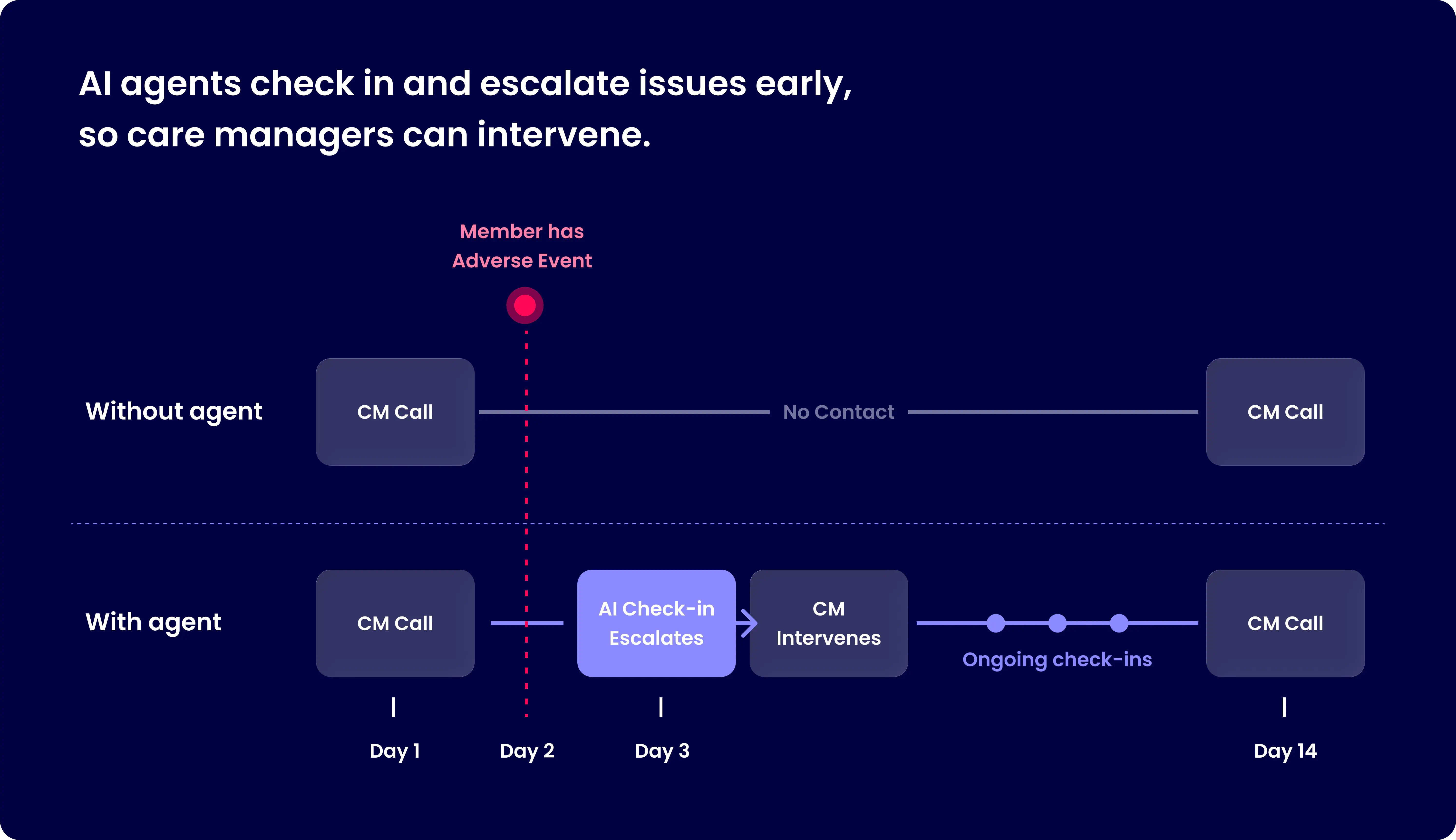
More touchpoints, stronger relationships
The counterintuitive insight: adding an AI agent doesn't reduce the human relationship — it strengthens it. Every check-in generates context that makes the care manager's next conversation more informed and more personal. The member feels more connected because someone is always noticing.
Instead of spending the first minutes of every call reestablishing context — How have you been? Any changes since we last spoke? — the care manager can start with what the agent already surfaced: I saw you mentioned trouble sleeping last week. Tell me more about that.
The agent handles the reach: check-ins, reminders, screenings, triage. The care manager handles the moments that require genuine human judgment. Every handoff is warm. Every escalation is informed. And the member never falls silent between sessions without someone noticing.
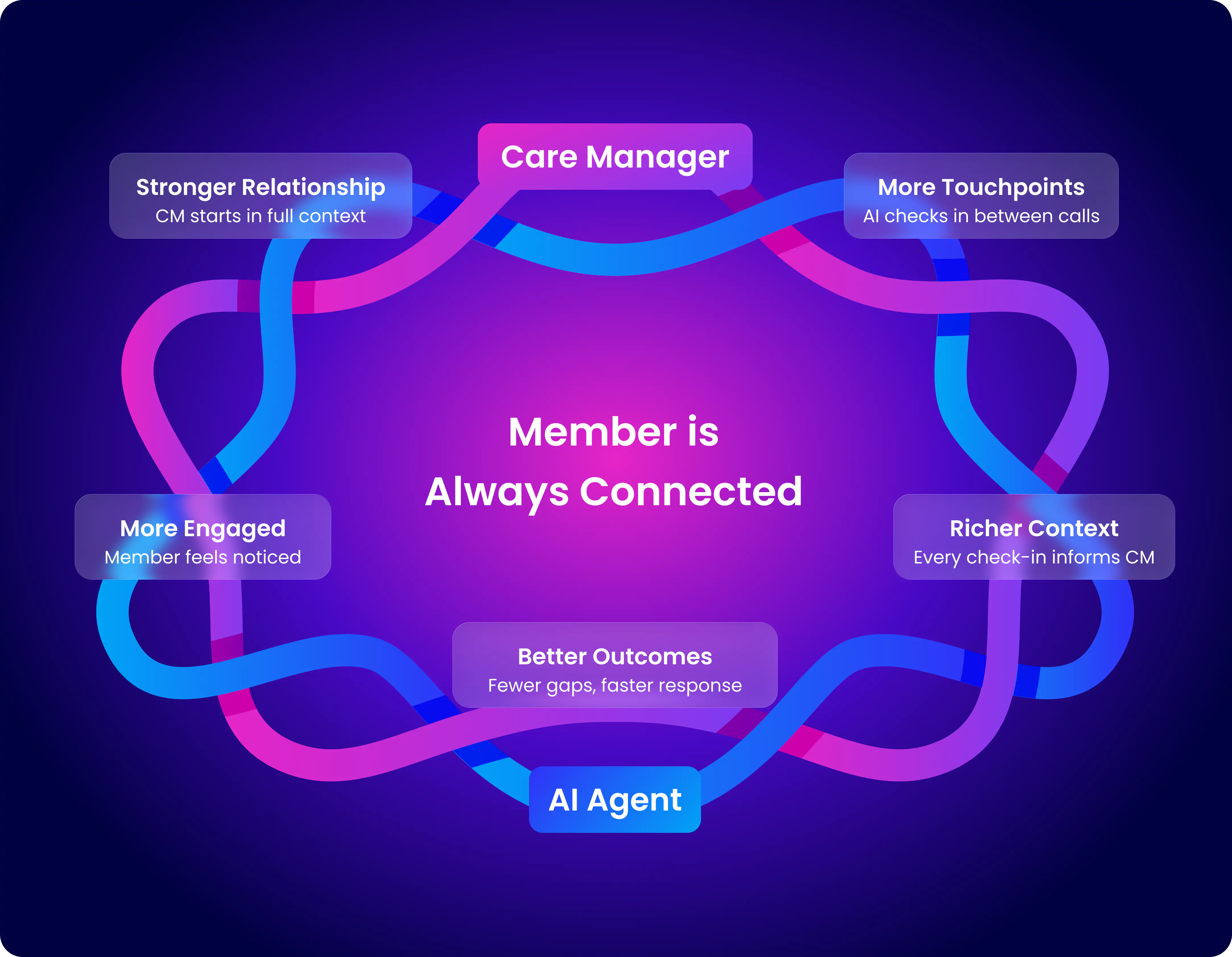
Care management, always connected
Healthcare built itself around the encounter because that was the only unit of care delivery available. Conversational AI fills in the space around it.
Members can be supported when they need it, not just when they're scheduled. Care managers can finally deliver the model they were trained for: real, sustained, human connection — at a frequency that actually changes outcomes.
That's not a small shift. It's care management, always connected.
Get in Touch 👋
Let’s talk about how Laguna can Elevate Your Care 💜 Team



%201.webp)